Peripheral Vascular Disease
What is Peripheral Vascular Disease?
Some other names used to refer to PVD are:
- arterial insufficiency of the legs
- claudication
- intermittent claudication
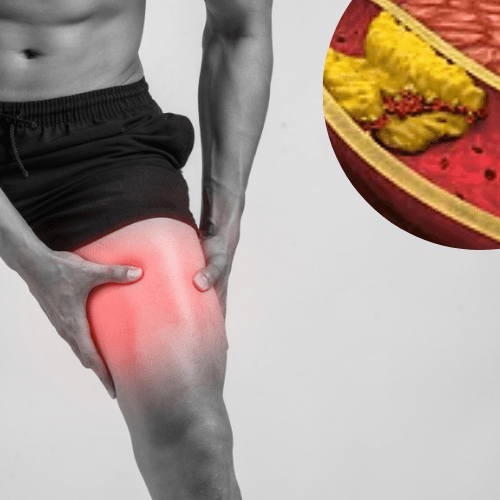
How do they develop?
Healthy peripheral arteries are stable and unobstructed, allowing blood to freely provide the legs with oxygen, glucose and other nutrients. However, as we age, the peripheral arteries build up plaque – a sticky substance made up mostly of fat and cholesterol. This sticky content narrows the passageway within the arteries and causes them to become stiff, which further restricts the free flow of blood to the organs and limbs. As plaque growth progresses, clots may develop and completely block the artery. If allowed to progress, this can lead to organ damage and loss of fingers, toes, or limbs. Notably, in PVD cases, the narrowing of blood vessels can be either caused due to Arteriosclerosis (i.e. hardening of the arteries) or blood vessel spasms. A moderate blockage in significant leg muscles, like the calf or thigh, may cause pain when walking that can temporarily decrease with rest but present again due to any kind of movement or activity.
What are the risk factors for PVD?
- don’t get enough exercise
- practice smoking
- are over age 50
- are overweight
- have abnormal/ high cholesterol
- have high blood pressure
- have diabetes
- have heart disease
- have a family history of Vascular problems
Book an Appointment For a Consultation
What are the causes of Peripheral Vascular Diseases?
Symptoms :
MAY HIDE: Many patients experience no symptoms.
- PAIN IN MUSCLES WHILE WALKING Pain in your muscles of the calf, thigh, hip, or buttock while walking (claudication) may signal you have PAD. Typically, the pain occurs after walking a certain distance and then goes away with rest.
- PAIN IN LEG WHILE SLEEPING If you have pain in the leg while sleeping, then it’s worrying as you may have an advanced case of PAD.
- BLACKENING OF TOES-GANGRENE Blackening of toes is called gangrene and means there is critical blockage of vessels. This is a part of the term called Diabetic foot & It requires immediate treatment.
- OPEN WOUND OR ULCER ON TOES An open wound or ulcer on your toes, often at a pressure point on foot, can signal a severe case of PAD. This is also a part of a term called Diabetic foot. An ulcer can progress to gangrene. These symptoms require immediate medical attention. Weakness Numbness or Pain in Toes or Feet Muscle Fatigue or Cramps Open Wounds on Feet
- Weakness
- Numbness or Pain in Toes or Feet Muscle Fatigue or Cramps
- Open Wounds on Feet
Why Us?
Treatment depends on the symptoms and findings on USG Doppler or angiography. If there is a critical blockage, then angioplasty & stenting may be required. In angioplasty, a balloon is inflated to open the vessel & if the needed stent is then deployed.
The patient is asked to be fasting 6 hours before the procedure. After the procedure is complete, the patient is observed overnight and discharged the next day itself. The patient can walk from the next day itself.
While it varies from hospital to hospital & depending on the number of balloons/stents that will be required, it usually is around 1.25 lakhs. Our experts will be able to give the expected budget after evaluating you.
From the very next day, the patient is able to walk after which s/he is advised to walk for 30 minutes to 1 hour every day. Patients are recommended to regularly take their medications, including blood thinners, diabetes, and blood pressure medications. Regular sugar & BP monitoring is a must. Also, follow-up, as advised by our experts, should be followed diligently.
Absolutely. The procedure of angioplasty is performed through a pin-hole & involves no cuts/sutures. The patient is, in fact, mobile from the next day itself. The procedure is done under local anaesthesia, and the patient is conscious during the entire procedure. At The Vascular Center, we believe in using the powers of music to help boost the spirits of our patients and healthcare staff. We in fact play music of the patient’s choice during the procedure, just to calm them down and decrease their stress.
